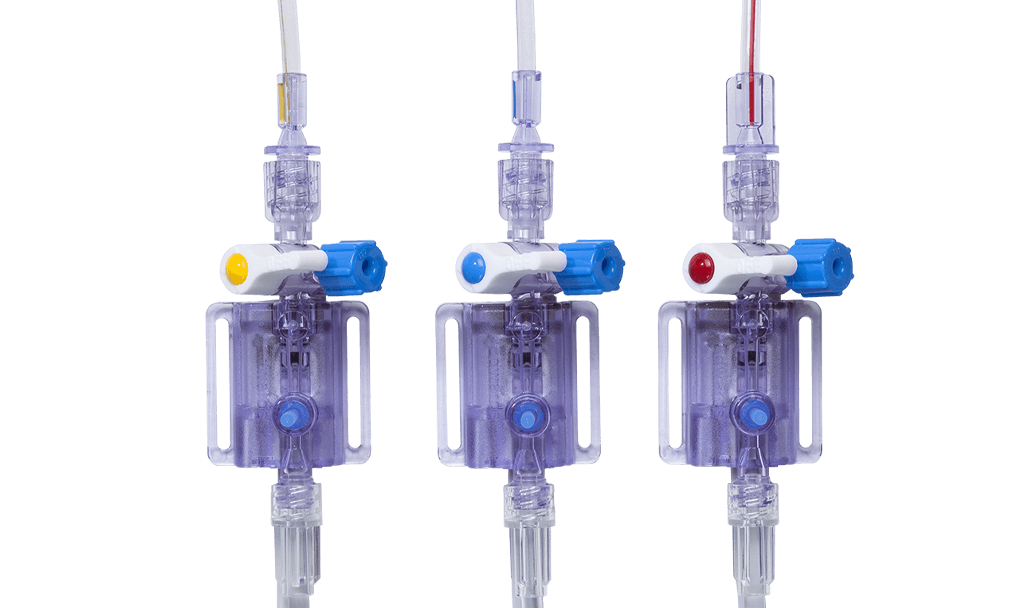
Closed blood sampling
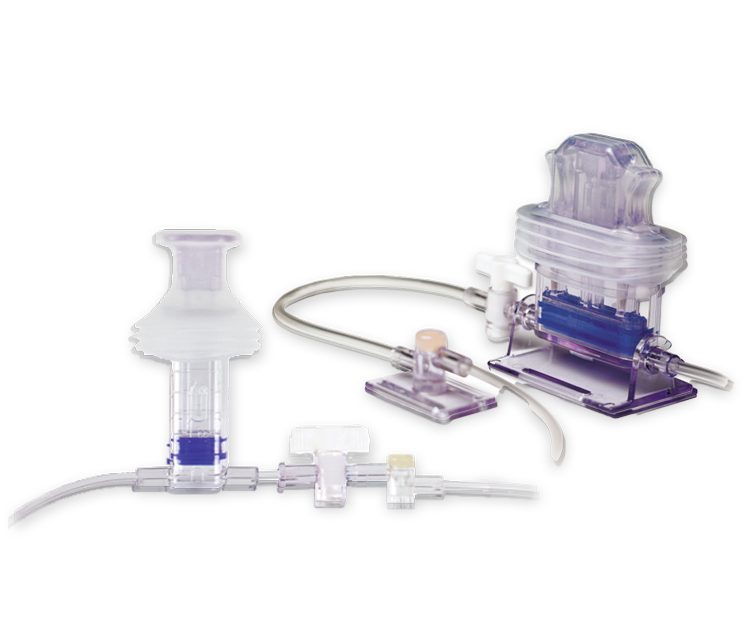

VAMP adult system
To minimize blood loss during sampling, Edwards Lifesciences' VAMP closed blood sampling systems incorporate an in-line reservoir that allows clinicians to reinfuse rather than discard the clearing volume. Needleless VAMP systems are designed to reduce infection, needle sticks, and blood waste associated with conventional blood sampling methods.1-4
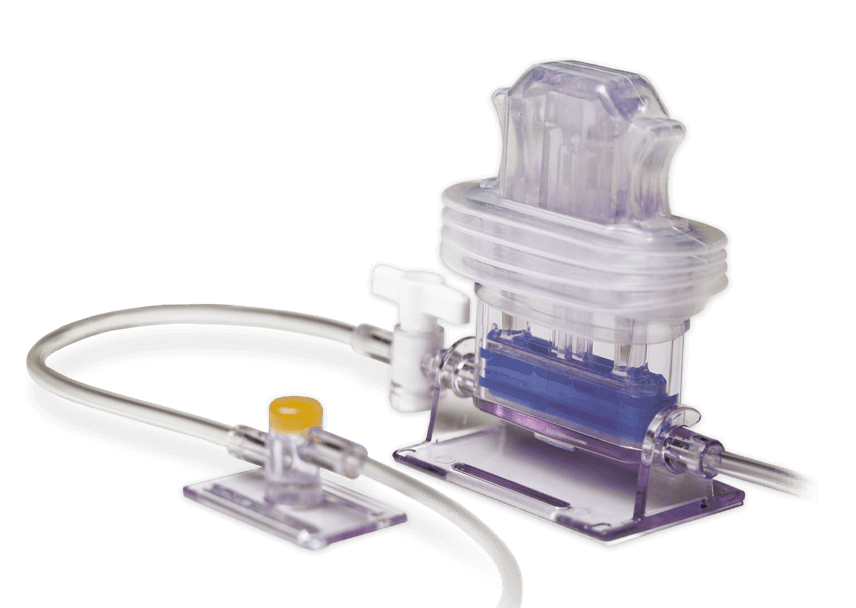
Safe, simple and reliable closed blood sampling for effective patient blood management.
- VAMP adult system is designed to reduce infection and blood waste associated with traditional blood sampling
- 5 cc reservoir designed for safe and convenient blood sampling in environments where close proximity to the patient is desired
- For use with disposable pressure transducers and for connection to central line catheters and arterial catheters
- Versatile design can be pole mounted on a backplate or used as an arm mount
- Z-site self-sealing sample port reduces blood buildup for collection of undiluted samples and improves infection control compared to traditional sampling methods
VAMP adult system setup video
This video details the process of setting up and drawing blood using VAMP adult system in conjunction with TruWave pressure transducer.
Model numbers
| Model | Description | Unit of measure |
| 48VMP106 | 6'' sampling kit, sample site, reservoir and two shut-off valves | CS(20) |
| 48VMP120 | 20'' sampling kit, sample site and arm-mount reservoir | CS(20) |
| 48VMP160 | 60'' sampling kit, sample site and arm-mount reservoir | CS(20) |
| 48VMP184 | 84'' sampling kit, sample site and arm-mount reservoir | CS(20 |
| 48VMP284 | 84'' sampling kit, sample site and pole-mount reservoir | CS(20) |
| 48AVMP | VAMP system anesthesia kit, 68'' sampling kit with male / female connector | CS(20) |
VAMP Plus system
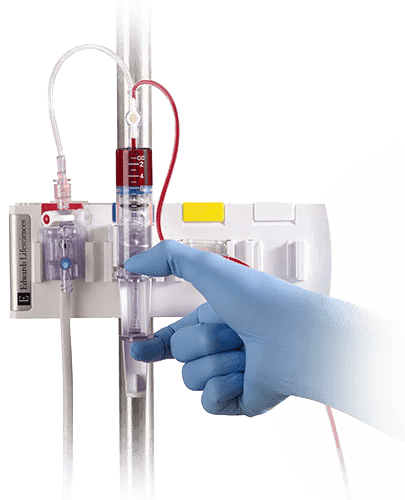
Sampling flexibility between surgery and intensive care
- Large 12 cc reservoir provides optimized clearing volume
- Choice of one or two Z-site sample sites for flexibility in perioperative settings
- Convenient one-handed operation simplifies sampling and clearing volume reinfusion
- For use with disposable pressure transducer kit or for individual connection to central line or arterial catheters
VAMP Plus system setup video
This video illustrates the process of setting up and taking a blood sample from VAMP Plus system when paired with TruWave pressure monitoring system.
Model numbers
| Model | Description | Unit of measure |
| VP1 | VAMP Plus system reservoir with 60 in (152 cm) patient tubing and one sample site located 55 in (140 cm) from the patient | CS(10) |
| VP2 | VAMP Plus system reservoir with 60 in (152 cm) patient tubing and two sample sites located 13 in (33 cm) and 55 in (140 cm) from the patient | CS(10) |
VAMP Jr system
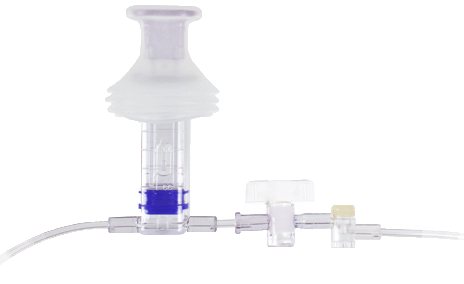
Safety and accuracy for your smallest patients
- Designed to meet the volume-critical requirements of pediatric patients
- Smaller 3 cc reservoir optimizes clearing volumes, providing undiluted, accurate blood samples
- Graduated “cc” markings aid in selecting appropriate clearing volume for each patient
- Special contamination hood helps reduce infection risk
- Variety of tubing lengths to accommodate patient size requirements
VAMP Junior system setup video
This video illustrates the steps involved with setting up and taking a blood sample from VAMP Jr system.
Model numbers
| Model | Description | Unit of measure |
| VMP306 | 6'' kit with 3 cc reservoir and 2 access sites | CS(20) |
| VMP406 | 6'' kit with 3 cc reservoir and 1 sample site | CS(20) |
| VMP426 | 26'' kit with 3 cc reservoir and 1 sample site | CS(20) |
VAMP Flex system
Sampling flexibility between surgery and intensive care on an offline system.
- Large 10 cc reservoir provides optimized clearing volume
- Choice of one or two Z-site sample sites for flexibility in perioperative settings
- Offline version
- Available individually or integrated into your disposable pressure transducer kit
Accessories
Model numbers
| Model | Description | Unit of measure |
| VMP400 | VAMP system needleless cannula | CS(200) |
References
- Peruzzi, W.T., et al., A clinical evaluation of a blood conservation device in medical intensive care unit patients. Critical care medicine, 1993. 21 (4): p. 501-6
- Oto, J., et al., Comparison of bacterial contamination of blood conservation system and stopcock system arterial sampling lines used in critically ill patients. American Journal of Infection Control, 2012. 40(6): p.530-4
- O'Hare, D. and R.J. Chilvers, Arterial blood sampling practices in intensive care units in England and Wales. Anaesthesia, 2001. 56(6): p. 568-71
- Tang, M., et al,. Closed Blood Conservation Device for Reducing Catheter-Related Infections in Children After Cardiac Surgery. Critical Care Nurse, 2014. 34(5); p.53-61
Medical device for professional use
For a listing of indications, contraindications, precautions, warnings, and potential adverse events, please refer to the Instructions for Use (consult eifu.edwards.com where applicable).